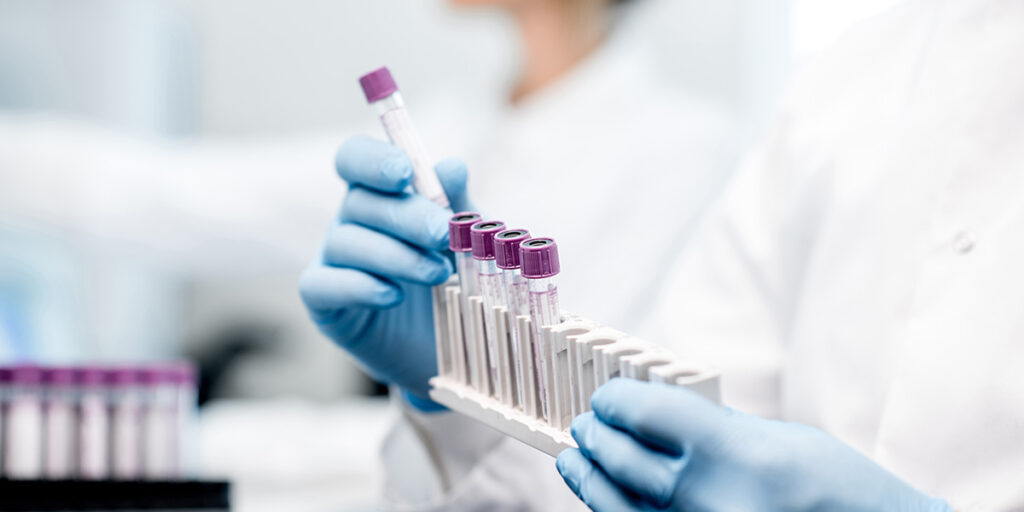
Recent Research Projects
Recent Research Projects
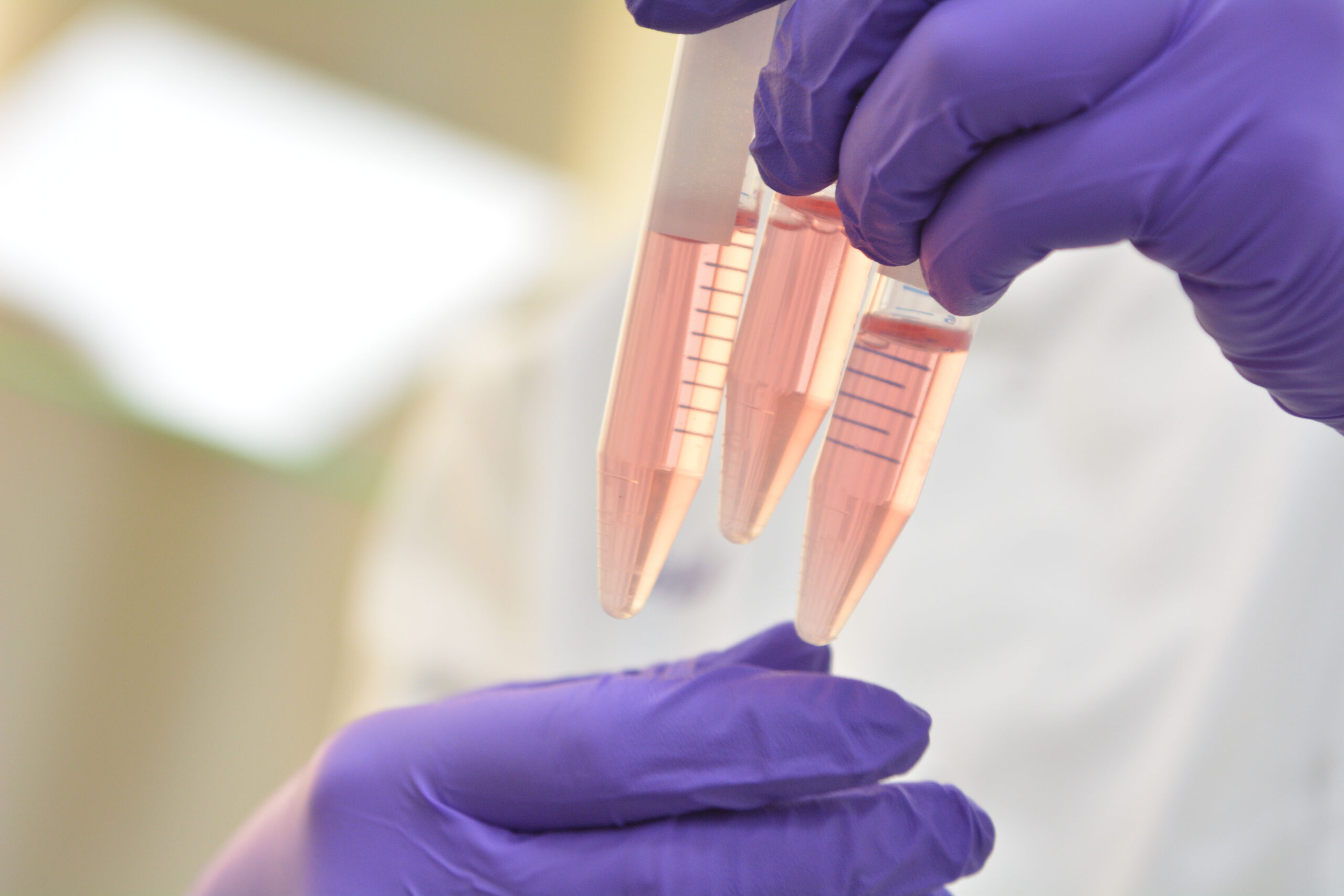
Wound Healing Solutions
At some point in their lives, around 4.5% of the UK population will have a wound that needs medical care. This not only impacts on the quality of their lives but also brings a massive economic burden to the NHS.
The Griffin Institute is working on a variety of wound healing solutions that do not require refrigerated transport and storage, which will allow for easier distribution and application. They will enable people from different demographic and socioeconomic backgrounds to access treatment, promoting greater equality of care.
1. Burn Injuries:
Burn injuries are a major epidemiologic issue worldwide. To treat burn injuries, there are three commonly used methods for wound treatment, however, there is a gap between supply and demand of required tissue and there can be serious clinical complications such as graft rejection.
To overcome this issue The Griffin Institute is working on an off the shelf epidermal product using components which are already present in the skin. It takes the form of a semi-solid gel that can be applied directly to a burn and “fixed” with a UV light to create a dressing with the ability to regenerate skin whilst protecting the wounds.
2. Cell Derived Scaffold for Skin Repair:
There are no ideal skin replacement products on the market. The structural and mechanical features of current skin products are very different from normal skin and are one of the major reasons for their failure. To overcome these issues we are developing an autologous[1], cell free, off the shelf epidermal scaffold orchestrated by reverse engineering[2]. In this first phase of the project, we will develop a scalable prototype of the epidermal and dermal scaffold by layering cells in different ratios.
3. Dermal Paste:
The cost of chronic wound care is estimated to consume at least 6% of NHS expenditure in the UK, and unfortunately many people are still left with wounds that simply will not heal using current treatment options that may cause distress and very poor quality of life. The Griffin Institute has developed a skin substitute that have been shown to accelerate wound closure.
This research has benefit across many areas, including pressure sores, surgical lacerations and wounds in children and older people who may be unable to tolerate the process of more traditional skin grafts. We have completed the first phase of research on our new wound healing solution, ‘Dermal Paste’, and are now working on pre-clinical trials.
4. Diabetic Wounds/Ulcers:
These are a common complication of diabetes that cannot be managed through diet, exercise, and insulin treatment, and can be extremely difficult to heal. Our skin replacement enriched with healing proteins collected from the patient’s own blood, stimulates the cells within the dermis (middle) layer of skin to lay down new matrices that are essential for wound healing.
[1] Using cells or tissues obtained from the host individual
[2] Reproduction following a detailed examination of the original construction/composition (in this case skin)
Wound Healing Solutions
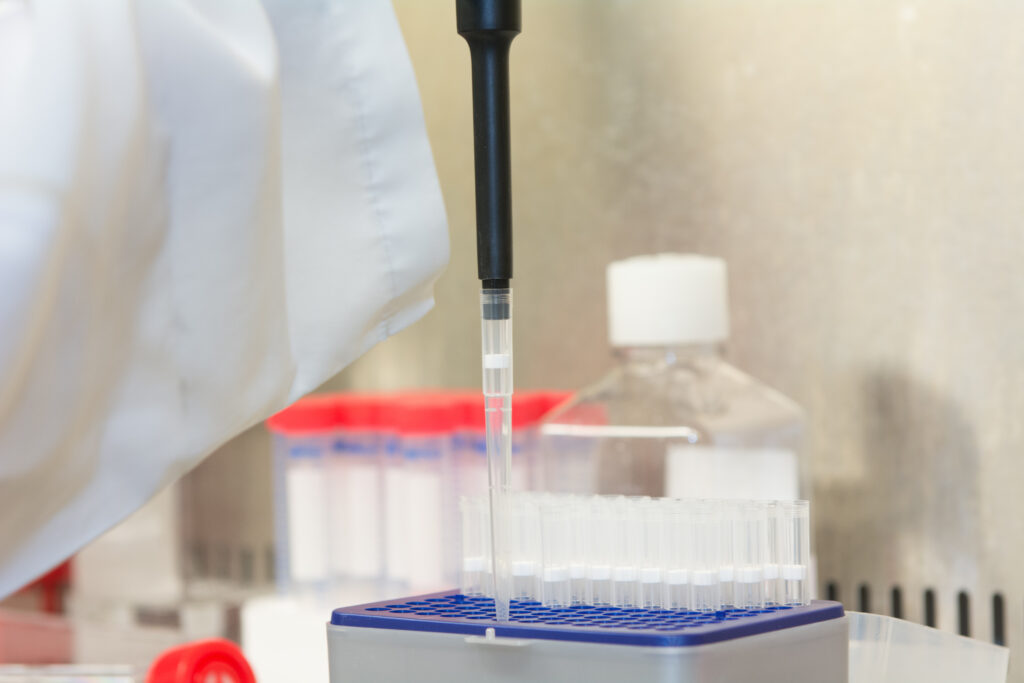
Intestinal Failure
Intestinal Failure (IF) such as Short Bowel Syndrome (SBS) or Crohn’s disease, and congenital malformations of the bowel, is a long-term and complicated disorder that causes malfunction to an extent where necessary nutrients, water and electrolytes cannot be absorbed efficiently. Patients with SBS, where half or more of the small intestine is removed, may suffer extensive physical and psychological consequences that can significantly affect their quality of life.
Patients with IF require intravenous supplementation, consisting of essential nutrients to maintain health and growth. Those who can no longer tolerate this, including children with congenital and irreversible IF, require a lifesaving bowel transplant. However, standard bowel transplants are limited due to the shortage of donor organs and poor survival outcomes, as well as a graft rejection rate of approximately 60%.
We are currently working with St Mark’s Hospital on generating bio-engineered bowel tissue, combining human decellularised intestine, seeded with patient-specific cells, which can be surgically transplanted onto the patient’s remaining intestine and thereby restore full function of the bowel.
Intestinal Failure
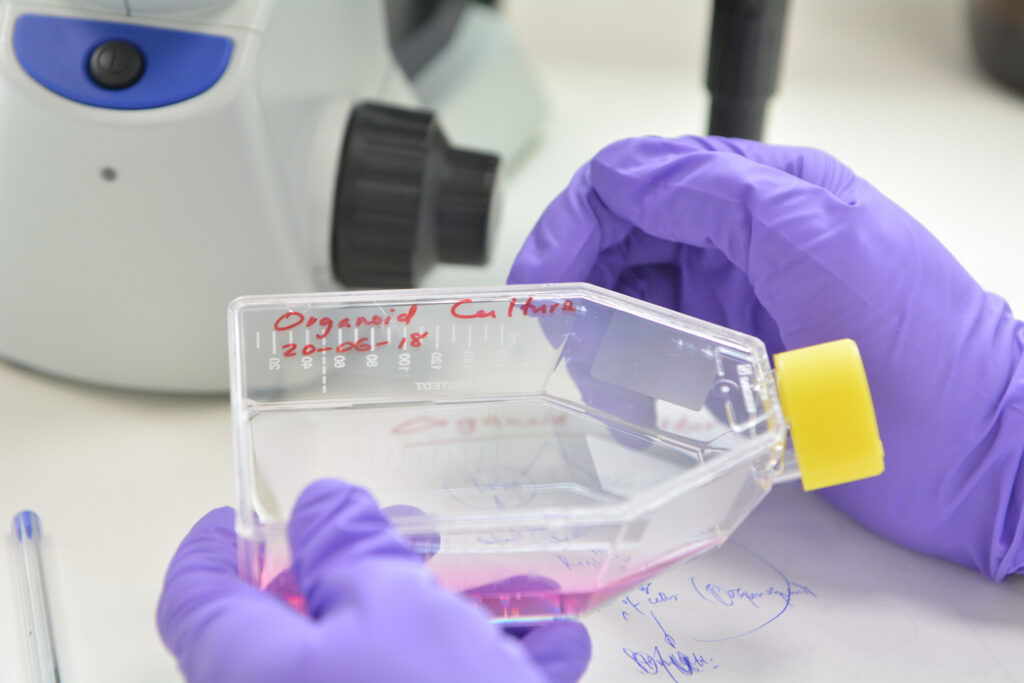
Breast Reconstruction Project:
Approximately 50,000 women are diagnosed with breast cancer each year in the UK, around 40% of whom will undergo a mastectomy. Current methods for breast reconstruction involve the implantation of synthetic material, which can have serious complications including infection/illness, immuno-compatibility and graft/implant failure.
The Griffin Institute is working to develop a breast implant from natural proteins, which are already present in the breast and will be used in conjunction with the patient’s own fat and stem cells. As the breast tissue grows, the implant will be absorbed, leaving behind a natural breast made with the patient’s own body tissue. This project is in an advanced stage and we are seeking investment towards the next phase of bringing it to patients.
Breast Reconstruction Project:

Orthopaedics:
1. Bone-tendon Graft:
Tendon rupture is a common clinical problem. This injury is usually painful and can seriously affect the ability to walk. Surgical repair is a standard care but challenging, hence The Griffin Institute is developing an off the shelf novel solution for bone-tendon junctions, for better surgical outcomes.
2. Hip Replacements:
These are among the most successful surgeries in improving patient quality of life. However, revision hip replacements due to loosening of the implant and bone defects, account for 10% of surgeries, adding extra burden to the NHS and causing adverse impact on the patient’s life. The Griffin Institute continues to research methods on regenerating new bone, to improve clinical performance and prevent future problems.
Orthopaedics:
Urethral Strictures
These are a narrowing of the urethral lumen which can progress to urinary tract obstruction and complications such as urinary retention, infection, stones, and renal failure. Urethral stricture disease is the most common cause of lower urinary tract symptoms in men, with an estimated prevalence of 10 per 100,000 in men in their 20’s and 100 per 100,000 in men over 65. Current standard treatments are unsatisfactory due to very high recurrent stricture rates or significant adverse events from open surgery, demanding long recovery time with associated problematic long-term complications.
There is an unmet clinical need for an alternative stricture treatment to improve on stricture recurrence rates and ideally effect a cure. We are working on a project to use stem cells to transform the management of urethral stricture disease, with pre-clinical evidence showing that this supports the healing process with reduced recurrent stricture rates. We now require funding for necessary proof-of-concept study to fulfil regulatory requirements prior to proceeding to clinical trials.
Urethral Strictures